Breast cancer is one of the most common cancers among women and is the second leading cause of death. This means all women are at risk for breast cancer and should be proactive in maintaining breast health. According to the National Breast Cancer Coalition, only 5 - 10% of those with breast cancer have inherited a gene mutation for breast cancer and 90 - 95% of breast cancer cases involve inherited mutations. That means that even without the presence of a family history of breast cancer, you are still at risk for developing it. For those who have been diagnosed with early-stage breast cancer, a breast cancer lumpectomy is recommended.
What Is a Lumpectomy?
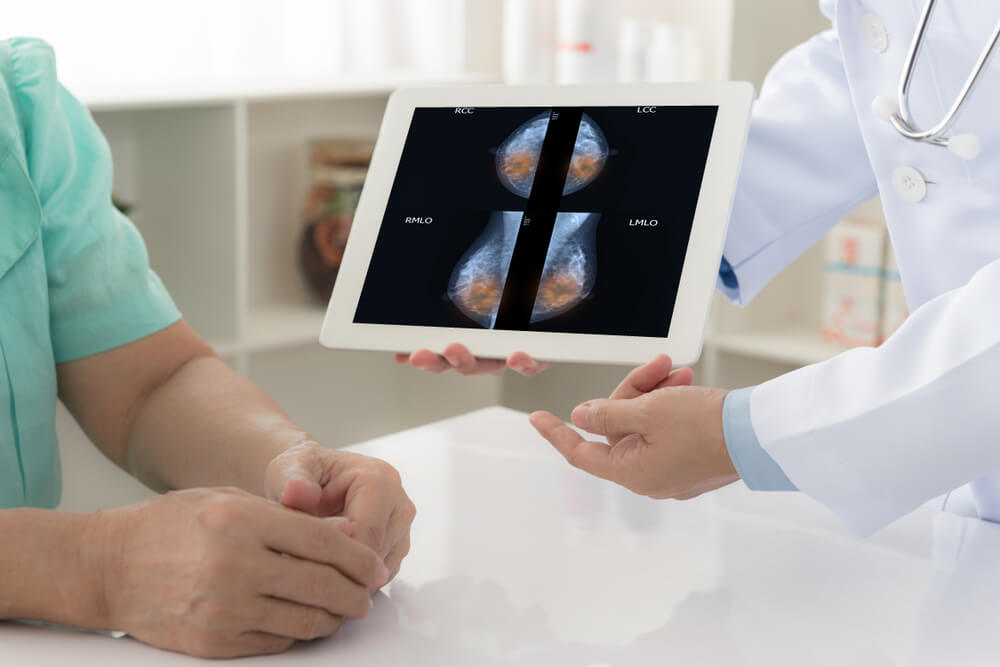
A lumpectomy is a surgical procedure in which a lump is removed from the breast containing breast cancer cells. This step is typically taken when the cancer cells are contained and have not spread. It is a kind of partial mastectomy that is referred to as a breast saving surgery since it allows patients to keep most of their breast tissue. Lymph nodes under the arms may be removed, as well as parts of the chest wall lining if cancer is near it. Studies dating back to the 1970s have shown that lumpectomy along with radiation used to treat women with breast cancer had the same survival rates as mastectomy. Currently, 60% of women diagnosed with early stages of breast cancer, lumpectomy and radiation are recommended methods of treatment with high survival rates.
If you get a lumpectomy, you’ll most likely be able to return home the same day. Some who receive treatment chose to have local numbing anesthesia rather than general anesthesia. Women who received this type of treatment:
- Small single tumor - Women who have been diagnosed and have a small single tumor less than 5 centimeters in diameter are more likely to be recommended a lumpectomy.
- Enough tissue - Those who have enough tissue surrounding the tumor are recommended a lumpectomy since removing it won’t result in a misshapen breast.
- Medically fit - Women who are recommended lumpectomy treatment are medically able to handle the surgery and follow up radiation treatment.
It’s important to note that having a lumpectomy is not an option for everyone. There are some instances that can prevent women with early stages of breast cancer from receiving this treatment. Below are cases where a lumpectomy is not recommended:
- Scleroderma - This is a condition that makes tissues harden. After a breast lumpectomy, the tissues in your breast are likely to harden with this condition.
- Lupus - This is an inflammatory illness that will worsen with radiation treatment.
- Previous radiation - If you’ve already had radiation treatment on your breast, it is too risky to repeat the treatment again.
- Cancer - If cancer has spread throughout the breast and the skin over it, lumpectomy treatment will not be able to address it all. A different form of treatment will be necessary.
- Large tumor - If you have a large tumor and small breasts, a breast lumpectomy will not be recommended.
- More than one - If there are two or more tumors in the breast, a surgeon will not be able to remove all of cancer with one cut. This means that more than one cut can make the breast look awkward and lumpy after a breast lumpectomy.
- Access - If you have no access to radiation treatments, a lumpectomy will not be recommended.
- Pregnancy - If you are pregnant, a breast lumpectomy would not be advised.
- Prior to breast cancer - If you’ve had radiation treatment on the same breast, a lumpectomy would not be recommended.
- Difficulty - If you have a tumor in an area where it would be hard to remove the surrounding tissues, a breast lumpectomy and radiation would not be recommended.
What to Expect During a Breast Lumpectomy
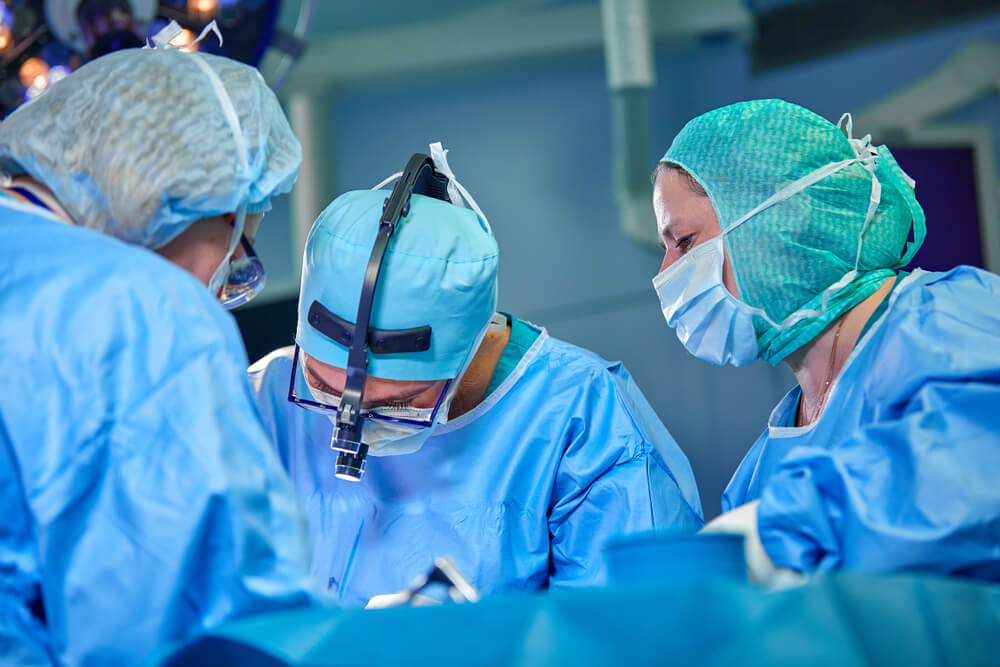
Before the day of your lumpectomy, your surgeon will give you specific instructions to follow, an overview of the procedure, and recommended recovery and aftercare procedures. The operation usually takes an hour or two and the doctor will have you change out of your clothes into a hospital gown. You’ll wait in a preoperative area until they are ready to begin the surgery. In the event the surgeon can’t find your tumor before the surgery, they will use a procedure to locate and mark the tumor using a mammogram or ultrasound. They will make markings on the breast with a marker to show where the incisions will be made before they begin. After they’ve decided where they will make the first cut, you will be taken to an anesthesia room where the nurse will begin the anesthesia through an IV into your hand or arm. Again, many people chose a local anesthetic.
- During surgery - The surgery should take no more than 40 minutes. The surgeon typically makes a curved incision using an electric scalpel that utilizes heat to minimize bleeding. If the tumor can easily be seen and felt, the surgeon will immediately remove it and some of the peripheral tissue around it. They will sometimes inject a rubber tube into the breast to drain the fluid that has accumulated in the space where the tumor was removed. The wound will be closed using stitches.
- After surgery care - Once the incision is close and you are removed from the surgery room, medical staff will monitor your vital signs. You’ll be able to go home unless you have lymph nodes removed. In this case, you may have to stay overnight. The nurse will give you information on home aftercare post-surgery that includes the following items:
-
- Prescriptions - Along with pain medication given in the recovery room, you may be prescribed medicine for home care. Even if you feel you may not need the medication, it’s still good to have on hand while in recovery.
-
- Stitches healing stages - It’s best to ask your surgeon how to take care of your bandage. Most likely, they will recommend a follow up so they can remove it themselves. If a surgical drain was placed, it may be removed before you go home. However, they may send you home with it for a couple of weeks. This will have to be drained a couple of times a day. Many surgeons use sutures that dissolve over time so there won’t be a need to remove them. If staples were used, your surgeon will take these out on the first visit.
-
- Exercise - It’s important to exercise your arm to avoid stiffness on the side you had a lumpectomy. The surgeon will recommend a routine that will start the morning after surgery. Other exercises won’t be recommended until drains are removed. Remember to always ask your surgeon any questions for additional clarity!
-
- Avoid infection - The surgeon should provide details on recognizing an infection and when to call.
- Recovering at home - Remembering to rest after the surgery is important to allow your body to recover. Taking the recommended medications should also help the healing process along. If you’ve had drains placed, take sponge baths until your doctors approve showers. Comfort during this phase is a priority so opt for wearing a sports bra regularly to avoid any movement of your breasts. In the weeks and months after the breast cancer lumpectomy, you may feel itchy or sensitive to touch. This is a normal part of the healing process that is sometimes managed with ibuprofen or opioids.
Request an Appointment Today
There are numerous factors that can increase a woman's risk of breast cancer. However, it’s important to remember that all women are at risk and should take steps to conduct regular screenings. If you have been diagnosed or would like more information on starting regular breast cancer screenings, give us a call. Our board-certified medical staff is here to support you on your health journey every step of the way. We are committed and passionate about providing personalized medical care to our family of patients.
Request your appointment today!





Leave A Comment
You must be logged in to post a comment.